Powerful Solutions For Increasing Your Practice’s Bottom Line
We provide healthcare organizations with solutions designed to optimize efficiency and maximize revenue so physicians and care providers have more time to focus on patient care.

Featured in USA Today | 2026
Revolutionizing the way your practice does business.
Revenue Cycle Management
Coding & Auditing
Credentialing
Consulting & MSO
HR and Staffing
Streamline Your Revenue Cycle Operations
Achieve Maximum Reimbursement
Empower your practice with Optimax’s expert solutions to expedite cash flow and enhance overall financial performance. Our tailored strategies streamline revenue cycle management, reduce administrative burdens, and help your team focus on delivering exceptional patient care. With Optimax, you gain a trusted partner committed to maximizing efficiency and supporting sustainable growth.
Core Services:
Empower your practice with Optimax’s expert solutions to expedite cash flow and enhance overall financial performance. Our tailored strategies streamline revenue cycle management, reduce administrative burdens, and help your team focus on delivering exceptional patient care. With Optimax, you gain a trusted partner committed to maximizing efficiency and supporting sustainable growth.
Revenue Cycle Management
Staff Augmentation
Credentialing
MSO Services
Human Resources
Coding Audits
Find Out How With Our Free Assessment
Ready to optimize your revenue? Achieve your maximum reimbursement by submitting the form below or calling our team at (888) 959-1014

Optimized Solutions for Healthcare
Efficient Revenue Cycle Management
Healthcare organizations today face rising costs, shrinking reimbursement, and staffing shortages that strain both operations and care quality. Optimax provides revenue cycle management and consulting solutions that streamline processes and strengthen financial performance. We manage the administrative complexities so your team can stay focused on delivering exceptional patient care.
Provide a dedicated client management team.
Handle patient interactions with understanding and compassion.
Use analytics to drive near real-time decisions and troubleshooting.
Empowering Your Success with Digital Strategy
Data That Drives Decision Making
Data should do more than report the past, it should power what’s next. At Optimax, we transform raw operational and revenue cycle data into clear, strategic direction.
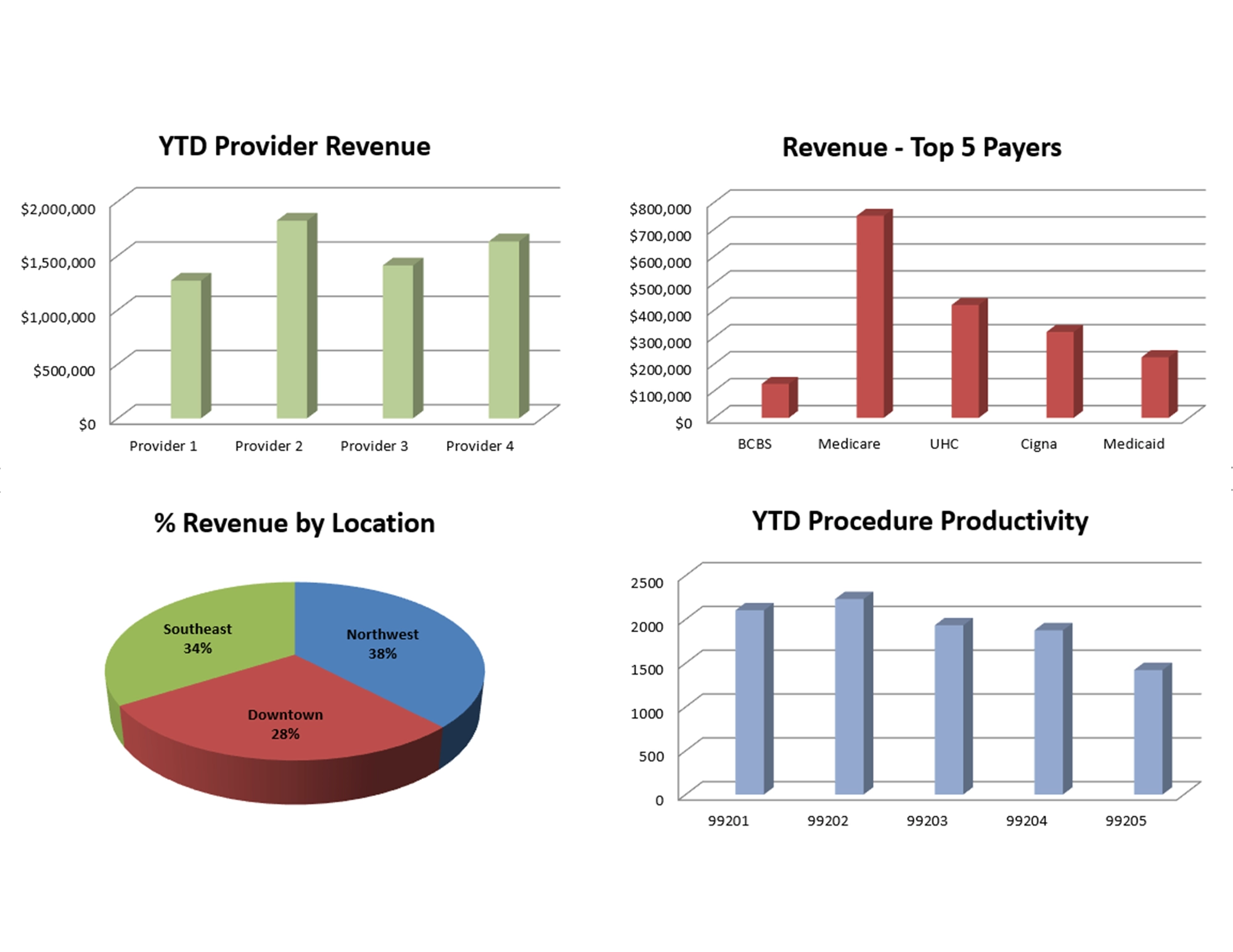
Real Time Analytics
Optimax delivers real-time analysis that gives leadership immediate visibility into revenue performance, payer trends, operational bottlenecks, and staffing efficiency.
Proven Results. Trusted by Healthcare Professionals
Healthcare professionals rely on Optimax to strengthen operations, maximize revenue, and position their organizations for sustainable profitability. The result is greater confidence at the executive level and stronger performance across the board.
Raymond Shaheen
We could not be more pleased with our Optimax partnership. Optimax has not only improved our financial outcomes but also led to better patient satisfaction. By simplifying billing and providing clearer patient statements, we’ve minimized confusion and complaints.
Joe Handy
“I recently had the pleasure of working with Optimax Billing and Consulting for our medical practice, and I can confidently say they’ve been a game-changer! Their team demonstrated unparalleled expertise in revenue cycle management, streamlining our billing processes with precision and efficiency. From accurate coding to swift claims processing, Optimax ensured our reimbursements were maximized and denials were significantly reduced.”